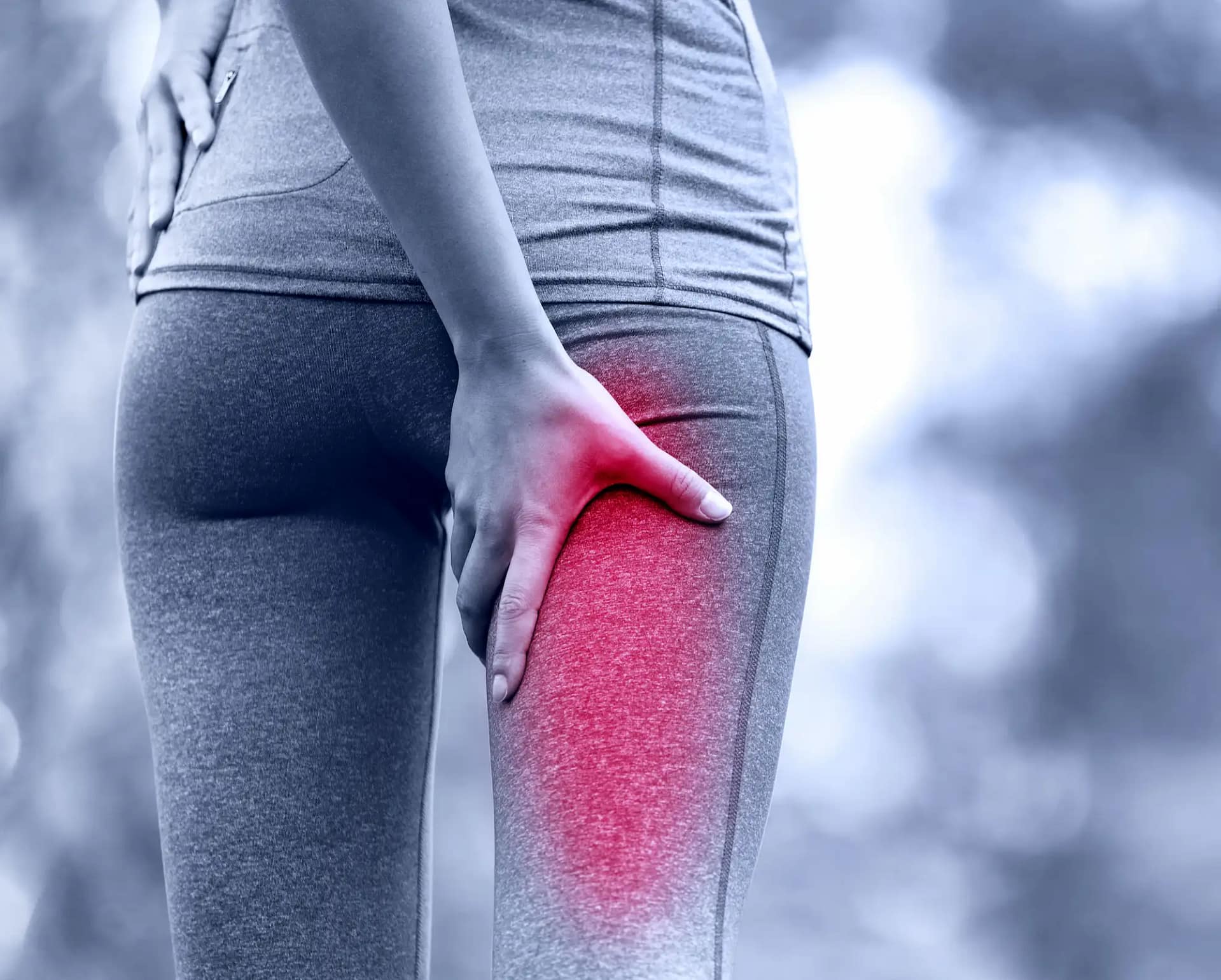
There’s a specific kind of misery to sciatica that people who haven’t had it can’t quite picture.
It’s not just the pain — it’s the way it travels. Starting somewhere in the lower back or buttock, it moves down the back of the thigh, sometimes all the way into the calf or foot, sometimes with burning, sometimes with a deep ache, sometimes with pins and needles that make you wonder if your leg is about to stop working altogether. Sitting makes it worse. Standing up from sitting is often the worst moment of the day. Long drives become an exercise in gritted teeth. Sleep, when it comes, is a relief — until you roll over and the whole thing starts again.
If that sounds familiar, you’re not alone. Sciatica is one of the most common musculoskeletal complaints in Australia, affecting up to 40% of people at some point in their lives. And yet it remains one of the most poorly managed conditions in the standard healthcare system — often treated with painkillers and a referral to wait-and-see, when the actual solution is considerably more direct.
At Advanced Health in Preston, sciatica is one of the conditions we treat most frequently. This post is our attempt to explain what’s actually happening in your body when you have it, why so many people struggle to get lasting relief, and what a proper chiropractic assessment and treatment plan can do that rest and medication simply can’t.
Sciatica Is a Symptom, Not a Diagnosis
This is the most important thing to understand — and the thing most people are never told.
When your doctor writes “sciatica” on a referral or a scan request, they are describing what you are experiencing: pain travelling along the sciatic nerve. They are not telling you why. The why matters enormously, because sciatica has multiple distinct causes, each of which responds to different treatment. Treating them all the same way — which is what happens when you’re simply given pain relief and told to rest — is why so many people spend months or years cycling through treatments that don’t work.
The sciatic nerve is the longest and widest nerve in the human body. It forms from several nerve roots in the lower lumbar spine (L4, L5) and sacrum (S1, S2, S3), merges into a single nerve trunk that runs through the buttock, and then travels down the back of each leg, splitting into smaller branches that supply sensation and motor function to almost the entire lower limb. When any part of this nerve is compressed, stretched, or irritated — anywhere along that path — the result is the familiar radiating pain, numbness, or weakness that we call sciatica.
The question, then, is what is doing the compressing or irritating. That’s where the clinical picture gets more nuanced, and where a proper assessment becomes essential.
The Four Main Causes of Sciatica
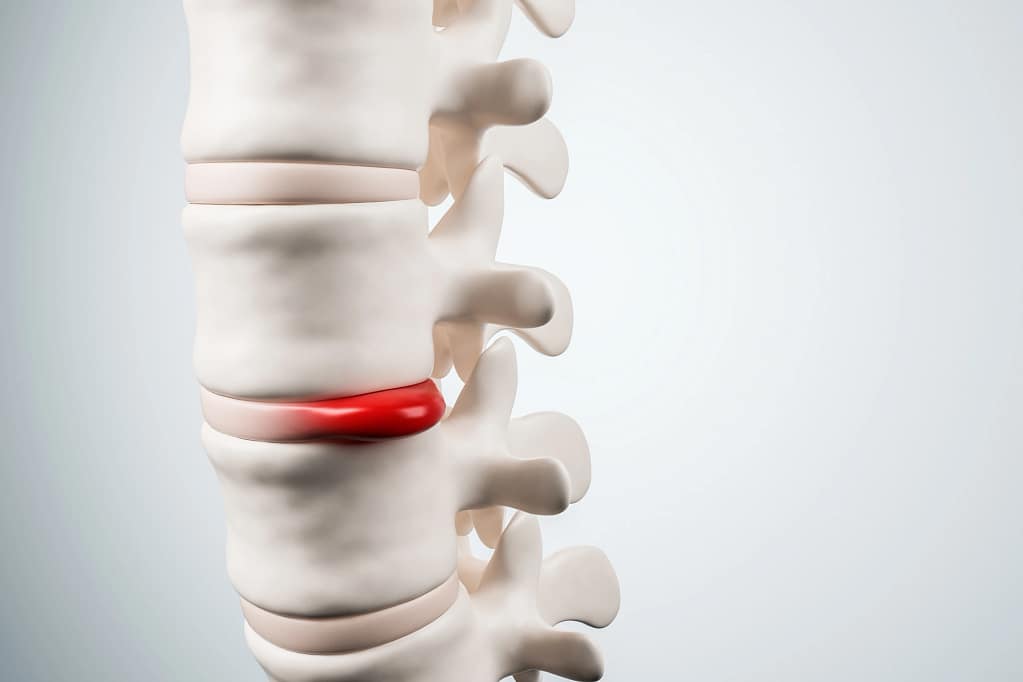
1. Lumbar Disc Herniation
This is the most common cause of true sciatica, accounting for the majority of cases. Between each pair of lumbar vertebrae sits an intervertebral disc — a structure with a tough outer ring (the annulus fibrosus) and a gel-like inner core (the nucleus pulposus). Under sufficient load or stress, particularly when the spine is repeatedly flexed under load (think: years of desk work, heavy lifting with poor mechanics, or sustained forward-bent postures), the outer ring can develop small tears. Over time, the inner nucleus can push through these tears and bulge outward — a disc herniation.
When the herniation occurs toward the back of the disc, near the exiting nerve roots, it can compress the sciatic nerve at its origin. This is classic disc-related sciatica: a very specific pain pattern that corresponds to the nerve root being compressed, often with associated neurological signs like weakness in specific muscle groups or reduced reflexes at the ankle or knee.
2. Piriformis Syndrome
The piriformis is a small but powerful external hip rotator muscle buried deep in the buttock. It lies directly over the sciatic nerve — and in approximately 15–20% of the population, the sciatic nerve actually passes through the muscle itself rather than beneath it.
When the piriformis becomes tight, hypertonic, or inflamed — as it often does in runners, cyclists, people with hip imbalances, and those who spend long periods sitting on hard surfaces — it can compress the sciatic nerve as it passes through or beneath it. The resulting pain is often mistaken for lumbar disc sciatica, but the distribution and character are subtly different, and the treatment is entirely different.
This distinction matters clinically. We see patients at our Preston clinic who have had extensive lumbar spine investigations — MRIs, CT scans, specialist consultations — that found nothing, because the source of their sciatica was never in the spine at all. It was sitting in the buttock the whole time.
3. Spinal Stenosis
Spinal stenosis refers to a narrowing of the spinal canal — the bony channel through which the spinal cord and nerve roots travel. This narrowing compresses the neural structures inside it, leading to pain, weakness, and sometimes the characteristic feature of stenosis-related sciatica: symptoms that worsen with walking or standing and improve with sitting or leaning forward (because flexion opens the spinal canal slightly, temporarily reducing the compression).
Stenosis is more common in middle-aged and older patients, and typically develops as a consequence of degenerative changes: bone spurs, thickened ligaments, and disc height loss that accumulates over years. It is manageable — often very effectively — with conservative care, though severe cases may require surgical consideration.
4. Sacroiliac Joint Dysfunction
The sacroiliac (SI) joints sit on either side of the sacrum at the base of the spine, connecting it to the pelvis. These joints absorb enormous force during everyday activities — walking, climbing stairs, getting in and out of cars — and when they become hypermobile, inflamed, or mechanically dysfunctional, they can produce a pain pattern that closely mimics lumbar or nerve-related sciatica: deep buttock pain with referral into the posterior thigh.
SI joint dysfunction is one of the most commonly missed diagnoses in lower back and leg pain. It accounts for an estimated 15–30% of chronic low back pain presentations, and it responds very well to targeted chiropractic manipulation and stabilising exercise.

What the Standard Medical System Gets Wrong About Sciatica
The conventional approach to sciatica — particularly in the early and acute phase — looks something like this: visit a GP, receive NSAIDs (anti-inflammatory medication) or muscle relaxants, possibly a short course of opioid-based pain relief, a referral for physiotherapy with heat and TENS, and instructions to rest. If symptoms persist, an MRI is ordered and a spinal specialist is consulted. Surgery — typically a discectomy or lumbar decompression — may be recommended.
The problem with this pathway is not that any individual component is wrong. It’s that the pathway treats sciatica as a monolithic entity rather than a collection of different conditions that happen to produce similar symptoms. It also relies heavily on passive treatments — medication, heat, rest — that address the experience of pain without addressing its structural cause.
Rest is particularly counterproductive for most sciatica. The lumbar spine and pelvis are dynamic structures that respond to movement. When we stop moving — when we lie still, avoid the activities that irritate us, and wait for the pain to settle on its own — we accelerate the very deconditioning and stiffness that makes the underlying problem worse. The muscles that support the lumbar spine weaken. The joints stiffen. The discs, which have no direct blood supply and rely on movement for nutrient exchange, become increasingly unhealthy. And the neural sensitisation that develops around chronic sciatica deepens.
The other significant gap in conventional management is the absence of a proper mechanical diagnosis. Imaging tells you what structural findings are present; it doesn’t tell you which of those findings are actually producing the pain. And clinical experience in musculoskeletal medicine makes it very clear that imaging findings and symptom severity often don’t correlate. Many people with bulging discs have no sciatica. Many people with severe sciatica have entirely normal-looking scans. The clinical assessment — how the person moves, what aggravates and relieves their symptoms, what neurological tests reveal — is what determines the real diagnosis.
How Chiropractic Care Addresses Sciatica
When you see a chiropractor in Preston or Thornbury for sciatica, the assessment is comprehensive and specific. We’re not guessing, and we’re not starting with a generic treatment protocol. We’re trying to establish, as precisely as possible, exactly what is producing your symptoms — and then treating that.
A thorough chiropractic assessment for sciatica includes:
Lumbar and pelvic assessment — examining joint mobility, segmental restrictions, and the mechanical behaviour of each lumbar level under various loading positions. This tells us where mobility is reduced, where there may be disc-related involvement, and how the spine responds to sustained postures.
Neurological testing — testing reflexes, sensation, and muscle strength in the lower limbs to identify whether there is genuine nerve root compromise and, if so, at which level. This is crucial information that shapes both the treatment approach and the urgency of care.
Hip and SI joint assessment — a set of provocative tests specifically targeting the sacroiliac joints, hip flexors, and piriformis to determine whether the source of the problem is in the pelvis rather than the spine.
Postural and movement analysis — because sciatica doesn’t exist in isolation. The way someone stands, sits, and moves through daily life has usually contributed to the problem, and understanding that mechanical picture is part of building a treatment plan that actually holds.
Once the cause is clear, treatment is targeted. For lumbar disc-related sciatica, spinal manipulation — applied at specific segments, in specific directions, with the right patient positioning — reduces the mechanical load on the disc and its surrounding structures, relieves muscle guarding, and begins to restore normal joint mobility. For piriformis syndrome, a combination of deep tissue release, dry needling (where appropriate), and hip mobility work often produces rapid improvement. For SI joint dysfunction, targeted manipulation to restore normal joint mechanics, combined with exercises to stabilise the pelvis, is reliably effective.
The goal is never simply to reduce pain in the short term. The goal is to correct the structural and mechanical reason the nerve is being irritated — and to give the patient a clear roadmap for keeping it that way.
What to Expect in Your First Few Appointments
People are often surprised by how much of the first visit is spent on assessment rather than treatment. That’s intentional. A correct diagnosis is the most important part of managing sciatica well — far more important than starting treatment quickly.
Your first visit at Advanced Health will typically include a thorough history of your symptoms (how they started, how they behave, what makes them better and worse), a detailed physical examination, and an initial treatment if appropriate. You’ll leave with a clear understanding of what we believe is causing your sciatica, what the treatment plan involves, and what to do at home in the meantime.
Most patients with acute sciatica from a lumbar disc herniation or SI joint dysfunction notice some change within the first two or three appointments — often a reduction in the distal symptoms (foot and calf) that signals the nerve is being decompressed. Full resolution typically takes longer, and the timeline varies depending on how long the condition has been present, the nature of the underlying cause, and how consistently the patient engages with the rehabilitative exercise component of care.
What we consistently find is that patients who combine hands-on chiropractic treatment with active participation — doing the prescribed exercises, modifying the aggravating activities, addressing the postural and ergonomic factors that contributed to the problem — recover faster and stay better longer than those who rely solely on passive treatment.
Managing Sciatica Day to Day: What Helps, What Doesn’t
While you’re working through treatment, a few practical principles tend to apply across most presentations:
Movement is medicine. Gentle, pain-aware movement — short walks, careful stretching, staying off the couch — is almost always better than bed rest. The exception is when neurological symptoms (significant weakness, loss of bladder or bowel control) are present, in which case urgent medical attention is warranted.
Ice over heat in the acute phase. Heat feels good on a sore back, but it increases blood flow and can exacerbate inflammation around an irritated nerve root. Ice packs applied to the lower back or buttock for 15–20 minutes at a time are more effective in the first 48–72 hours.
Avoid sustained sitting. If your job requires long periods at a desk, standing up every 30–40 minutes and taking a short walk is one of the most effective ways to manage disc-related sciatica during recovery. The disc pressure in sitting is significantly higher than in standing or walking.
Be careful with forward bending under load. For disc-related sciatica specifically, picking things up off the floor, loading the dishwasher, or gardening with a flexed lumbar spine can significantly aggravate the affected disc. Squat rather than hinge, and keep the back as neutral as possible.
We’re Here When You’re Ready
Sciatica can be genuinely debilitating — but it is also, in the vast majority of cases, highly treatable without surgery or long-term medication. The key is getting an accurate diagnosis and a treatment plan that addresses the actual cause rather than just the symptoms.
At Advanced Health in Preston, our chiropractors bring a thorough, evidence-based approach to sciatica — one that begins with understanding your individual presentation and ends with a plan to get you moving freely and keep you that way. Whether you’re in Preston, Thornbury, Reservoir, Northcote, or anywhere across Melbourne’s north, we’d love to help.
Book an appointment at advanced-health.com.au or call us on (03) 9484 9185.
We’re open 7 days — weekdays from 8am to 9pm, Saturdays from 7:30am, and Sundays from 9am.
4/107 Plenty Road, Preston VIC 3072
This post is for educational purposes only. If you are experiencing sciatica with progressive neurological symptoms — including new leg weakness, or any loss of bladder or bowel control — please seek urgent medical attention. For all other presentations, a thorough clinical assessment is the first and most important step.